妙佑医疗国际的方法
 妙佑医疗国际的腹腔镜肾脏切除术
妙佑医疗国际的腹腔镜肾脏切除术
妙佑医疗国际的外科医生在进行微创手术治疗以切除活体供体的肾脏(腹腔镜肾脏切除术)。
开始您的供体评估
单击此处填写病史问卷,开始活体肾脏或肝脏供体评估。
配对器官捐献
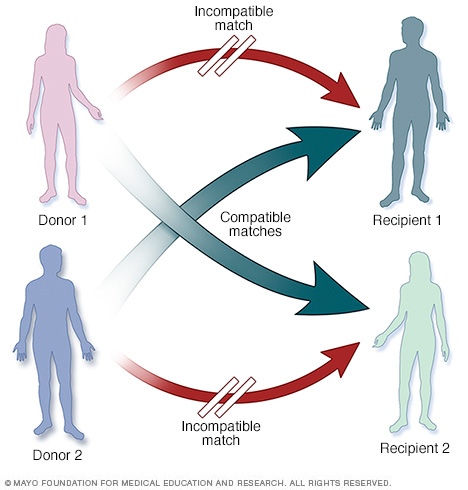
配对器官捐献
在配对器官捐献中,活体供体及其受体不相容,不能进行移植。但每对中的供体分别与另一对中的受体相容。如果供体和受体都愿意,医生可能会考虑配对器官捐献。
活体供体器官捐献链
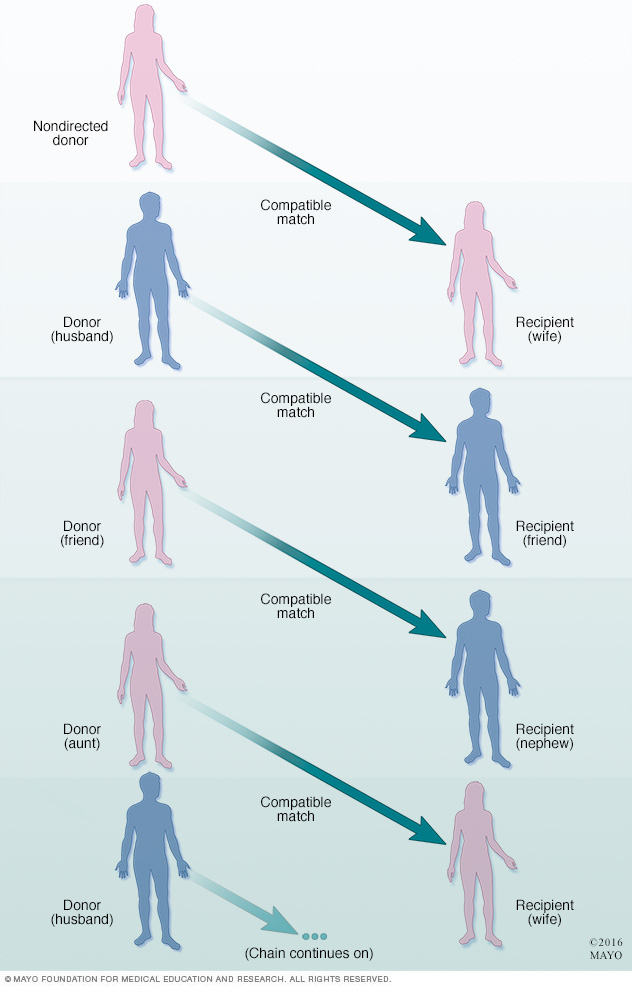
活体供体器官捐献链
为了得到匹配的器官,可以将一对以上不匹配的活体供体与受体与非定向活体供体联系起来形成一个捐赠链。
 医护团队角色
医护团队角色
受过不同医学专业培训的医务人员将以团队形式合作,以确保您的供体肾切除术取得良好结果。
专长与排名
 妙佑医疗国际的供体肾切除术会诊
妙佑医疗国际的供体肾切除术会诊
妙佑医疗国际拥有美国最大的活体肾移植项目之一。
经验
妙佑医疗国际在三地设有院区,其活体肾移植项目规模在全美名列前茅。妙佑医疗国际亚利桑那州、佛罗里达州和明尼苏达州院区每年进行数百例活体腹腔镜肾切除术和肾移植手术,其中包括许多复杂的外科类手术。
自 1963 年首次进行肾移植手术以来,妙佑医疗国际的肾移植外科医生目前已使用最先进的技术进行了 7000 多例手术。
妙佑医疗国际的肾移植团队在最复杂的肾移植方面具备丰富的经验,包括 ABO 不相容移植、交叉匹配阳性移植和配对捐献,还设有肾移植代谢项目。
先进的治疗方法和技术
妙佑医疗国际的外科医生具备关于所有类型的活体移植手术的丰富专业知识,包括微创手术、HIV 阳性器官捐献、配对器官捐献和其他复杂的手术。
创新和研究
妙佑医疗国际的移植研究人员走在领域前沿,致力于全方位地寻找新的、更好的移植方法,不断扩展移植的可用性,降低风险和改善移植结果。
我们的专家开创了多种手术方案,包括活体肾移植和透析前肾移植。
妙佑医疗国际移植中心为多项肾移植研究和活体器官移植研究提供支持。
全美公认的专业实力
妙佑医疗国际的肾脏移植结果优于全国平均水平。
位置、旅行和住宿
妙佑医疗国际移植中心为亚利桑那州、佛罗里达州和明尼苏达州的移植患者及其家属提供医护和住宿。
妙佑医疗国际的主要院区设于亚利桑那州凤凰城/斯科茨代尔、佛罗里达州杰克逊威尔以及明尼苏达州罗切斯特。妙佑区域医疗系统在几个州数十个地点均设有站点。
如果需要前来妙佑医疗国际就诊的更多信息,请在以下地点中进行选择:
费用与保险
活体捐赠者常问的费用与保险问题
了解更多信息
妙佑医疗国际有专门的移植经济服务代表和社工,可以为患者提供有关活体器官捐献的保险和财务方面的协助。
妙佑医疗国际与数百家保险公司合作,是数百万人的网络内医疗服务提供者。在大多数情况下,妙佑医疗国际不需要医生转诊。某些保险公司要求转诊,或有其它特定医疗要求。许多保险公司要求患者在接受移植服务之前先取得预先批准。
国际患者
妙佑医疗国际拥有专业的国际患者客户代表,他们可以帮助您解决与费用和保险有关的问题。阅读关于国际金融服务的更多信息。
Jan. 11, 2024
- KDIGO clinical practice guideline on the evaluation and management of candidates for kidney transplantation. Transplantation. 2020; doi:10.1097/TP.0000000000003136.
- AskMayoExpert. Living donor nephrectomy (adult). Mayo Clinic; 2020.
- About the kidney. Organ Procurement and Transplantation Network. https://optn.transplant.hrsa.gov/data/organ-datasource/kidney/. Accessed Aug. 23, 2021.
- National data: Donors recovered in the U.S. by donor type ⸺ Kidney. Organ Procurement and Transplantation Network. https://optn.transplant.hrsa.gov/data/view-data-reports/national-data/#. Accessed Aug. 23, 2021.
- Baez-Suarez Y, et al. Hand-assisted laparoscopic nephrectomy: Evaluation of the learning curve. Transplant Proceedings. 2020; doi:10.1016/j.transproceed.2019.10.010.
- O'Keeffe LM, et al. Mid- and long-term health risks in living kidney donors: A systematic review and meta-analysis. Annals of Internal Medicine. 2018; doi:10.7326/M17-1235.
- Wirken L, et al. Psychosocial consequences of living kidney donation: A prospective multicentre study on health-related quality of life, donor-recipient relationships and regret. Nephrology Dialysis Transplantation. 2019; doi:10.1093/ndt/gfy307.
- Suwelack B, et al. Investigation of the physical and psychosocial outcomes after living kidney donation ⸺ A multicenter cohort study (SoLKiD ⸺ Safety of Living Kidney Donors). BMC Nephrology. 2018; doi:10.1186/s12882-018-0871-z.
- Sharma V, et al. Living donor kidney transplantation: Let's talk about it. Clinical Medicine. 2020; doi:10.7861/clinmed.2020-0047.
- Yu ASL, et al., eds. Considerations in living kidney donation. Brenner & Rector's The Kidney. 11th ed. Elsevier; 2020. https://www.clinicalkey.com. Accessed Aug. 24, 2021.
- Living donation. United Network for Organ Sharing. https://unos.org/transplant/living-donation/. Accessed Aug. 24, 2021.
- Donate organs while alive. Human Resources & Services Administration. https://www.organdonor.gov/learn/process/living-donation. Accessed Aug. 24, 2021.
- What to expect after donation. National Kidney Foundation. https://www.kidney.org/transplantation/livingdonors/what-expect-after-donation. Accessed Aug. 25, 2021.
- Helpful tips for living donors and caretakers. National Kidney Foundation. https://www.kidney.org/transplantation/livingdonors/infotips. Accessed Aug. 25, 2021.
- About the operation: How to prepare for living donation transplant surgery. United Network for Organ Sharing. https://transplantliving.org/living-donation/about-the-operation/. Accessed Aug. 25, 2021.
- Find a transplant hospital: You have choices. United Network for Organ Sharing. https://transplantliving.org/before-the-transplant/find-transplant-hospital/. Accessed Aug. 25, 2021.
- Hart A, et al. OPTN/SRTR 2019 annual data report: Kidney. American Journal of Transplantation. 2021; doi:10.1111/ajt.16502.
- Kidney transplant. Scientific Registry of Transplant Recipients. http://www.srtr.org. Accessed Aug. 25, 2021.
- Guidance for the informed consent of living donors. Organ Procurement and Transplantation Network. https://optn.transplant.hrsa.gov/resources/guidance/guidance-for-the-informed-consent-of-living-donors/. Accessed Aug. 31, 2021.
- Dialysis. National Kidney Foundation. https://www.kidney.org/atoz/content/dialysisinfo. Accessed Aug. 31, 2021.
- Programs for donor/recipient pairs with incompatible blood types. National Kidney Foundation. https://www.kidney.org/transplantation/livingdonors/incompatiblebloodtype. Accessed Aug. 31, 2021.
- 42 CFR Part 482 Medicare program: Hospital conditions of participation: Requirements for approval and re-approval of transplant centers to perform organ transplants; Final rule. Centers for Medicare & Medicaid Services. https://www.cms.gov/Regulations-and-Guidance/Legislation/CFCsAndCoPs/transplantcenters. Accessed Sept. 9, 2021.
- Xiao Q, et al. Comparison of surgical techniques in living donor nephrectomy: A systematic review and Bayesian network meta-analysis. Annals of Transplantation. 2020; doi:10.12659/AOT.926677.
- Living donor surgery. National Kidney Foundation. https://www.kidney.org/transplantation/livingdonors/the-surgery. Accessed Sept. 9, 2021.
- 10 questions to ask before having an operation. American College of Surgeons. https://www.facs.org/education/patient-education/patient-resources/prepare/10-questions. Accessed Sept. 10, 2021.
- Dingli D (expert opinion). Mayo Clinic. Oct. 6, 2021.