Overview
Claudication
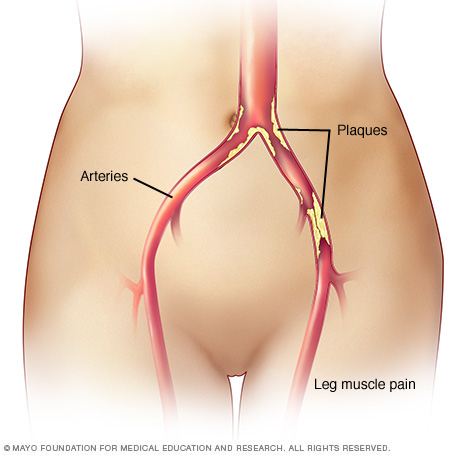
Claudication
Claudication is pain in the legs or arms that occurs while walking or using the arms. The pain is caused by too little blood flow to the legs or arms. Claudication is usually a symptom of peripheral artery disease, in which the arteries that supply blood to the arms or legs, usually the legs, are narrowed. The narrowing is usually due to a buildup of fatty deposits (plaques) on the artery walls.
Claudication is pain caused by too little blood flow to muscles during exercise. Most often this pain occurs in the legs after walking at a certain pace and for a certain amount of time — depending on the severity of the condition.
The condition is also called intermittent claudication because the pain usually isn't constant. It begins during exercise and ends with rest. As claudication worsens, however, the pain may occur during rest.
Claudication is technically a symptom of disease, most often peripheral artery disease, a narrowing of arteries in the limbs that restricts blood flow.
Treatments focus on lowering the risks of vascular disease, reducing pain, increasing mobility and preventing damage to tissues.
Products & Services
Symptoms
Claudication refers to muscle pain due to lack of oxygen that's triggered by activity and relieved by rest. Symptoms include the following:
- Pain, ache, discomfort or fatigue in muscles every time those muscles are used
- Pain in the calves, thighs, buttocks, hips or feet
- Less often, pain in shoulders, biceps and forearms
- Pain that gets better soon after resting
The pain may become more severe over time. You may even start to have pain at rest.
Signs or symptoms of peripheral artery disease, usually in more-advanced stages, include:
- Cool skin
- Severe, constant pain that progresses to numbness
- Skin discoloration
- Wounds that don't heal
When to see a doctor
Talk to your health care provider if you have pain in your legs or arms when you exercise. Claudication can lead to a cycle that results in worsening cardiovascular health. Pain may make exercise intolerable, and a lack of exercise results in poorer health.
Peripheral artery disease is a sign of poor cardiovascular health and an increased risk of heart attack and stroke.
Other conditions involving the blood, nerves and bones can contribute to leg and arm pain during exercise. It's important to have a complete exam and appropriate tests to diagnose potential causes of pain.
Causes
Development of atherosclerosis
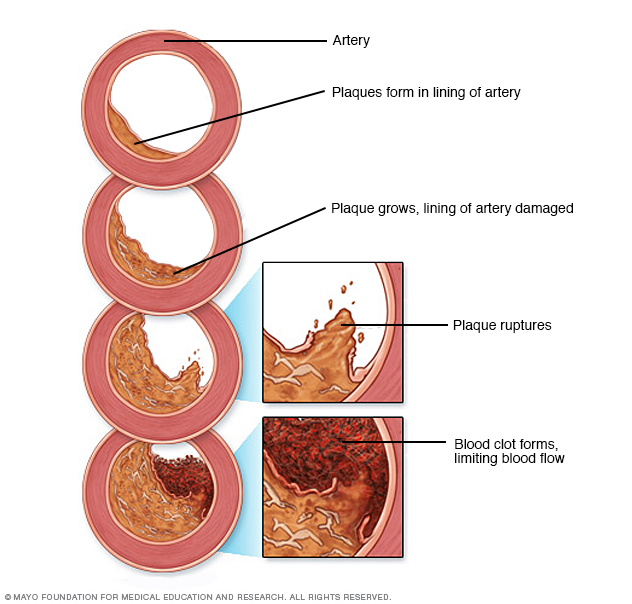
Development of atherosclerosis
If there's too much cholesterol in the blood, the cholesterol and other substances may form deposits called plaque. Plaque can cause an artery to become narrowed or blocked. If a plaque ruptures, a blood clot can form. Plaque and blood clots can reduce blood flow through an artery.
Claudication is most often a symptom of peripheral artery disease. The peripheral arteries are the large vessels that deliver blood to the legs and arms.
Peripheral artery disease is damage to an artery that restricts the flow of blood in an arm or leg (a limb). When you're at rest, the limited blood flow is generally enough. When you're active, however, the muscles aren't getting enough oxygen and nutrients to work well and remain healthy.
Damage to peripheral arteries is usually caused by atherosclerosis. Atherosclerosis is the buildup of fats, cholesterol and other substances in and on the artery walls. This buildup is called plaque. The plaque can cause the arteries to narrow, blocking blood flow. The plaque can also burst, leading to a blood clot.
Risk factors
Potential risk factors for peripheral artery disease and claudication include:
- A family history of atherosclerosis, peripheral artery disease or claudication
- Age older than 50 years if you also smoke or have diabetes
- Age older than 70 years
- Chronic kidney disease
- Diabetes
- High blood pressure
- High cholesterol
- Obesity (a body mass index, or BMI, over 30)
- Smoking
Complications
Claudication is generally considered a warning of significant atherosclerosis, indicating an increased risk of heart attack or stroke. Other complications of peripheral artery disease due to atherosclerosis include:
- Skin lesions that don't heal
- Death of muscle and skin tissues (gangrene)
- Amputation of a limb
Prevention
The best way to prevent claudication is to maintain a healthy lifestyle and control certain medical conditions. That means:
- Eat a healthy, well-balanced diet
- Exercise regularly
- If you have diabetes, keep your blood sugar in good control
- Maintain a healthy weight
- Manage cholesterol and blood pressure
- Quit smoking if you're a smoker